
Capnography for procedural sedation and analgesia in the emergency department. Wheatley I (2018) Respiratory rate 3: how to take an accurate measurement. 
Continuous oximetry/capnometry monitoring reveals frequent desaturation and bradypnea during patient-controlled analgesia. Canadian Agency for Drugs and Technologies in Health. Richardson (2016) Capnography for Monitoring End-Tidal CO2 in Hospital and Pre-hospital Settings: A Health Technology Assessment. Sullivan (2019) 5 things to know about capnography. Farquharson et al (2019) A systematic approach to capnography waveforms. Long (2016) Interpreting Waveform Capnography: Pearls and Pitfalls. Gelman (2013) Capnography outside the operating room. Noticing all 3 aspects of capnography interpretation, clinicians ensure they have all information required to make clinical decisions and intervene appropriately.ġ. Inspiratory downstroke: Is it sloping, steep, or prolonged?Ĭapnography use is increasing in different clinical settings as professionals understand the importance of detecting respiratory compromise quickly and with a high degree of sensitivity.B-C The expiration phase of the respiration cycle. A gradual decrease in end tidal carbon dioxide can occur during reduced metabolism, hypothermia. A-B The baseline, that is the level of minimum CO2 concentration, observed immediately after inspiration. A normal variant in pregnant women during anesthesia. Expiratory/alveolar plateau: Is it sloping, steep, or prolonged? End-tidal CO2 is the concentration of ETCO2 capnographic measured at the end of tidal volume expired (Point D in the above diagram).Expiratory upstroke: What is the shape? (i.e.Inspiratory baseline: Is there rebreathing?.Look for presence of exhaled CO 2: Is a waveform present?.Long (2016) suggests a systematic process to analyse capnography waveforms, divided into 5 steps: 2 3 Baseline, trend, frequency, shape, height, and width of the waveform all provide useful clues as to the quality of ventilation. These can possibly reduce errors of interpretation or clinical interventions. Systematic approaches to carbon dioxide waveform interpretation have been published. Phase IV: start of inhalation, CO 2 decreases to zero as atmospheric air enters the airway.This phase ends with a value of maximum CO 2 concentration Phase III: CO 2 concentration is relatively constant (reflects the concentration of CO 2 in the alveolar gas).Phase II: CO 2 increases rapidly as alveolar gas exits the airway.It demonstrates this graphically via the capnogram waveform. Phase I: start of exhalation, CO 2 concentration is initially zero Capnography is the measurement of the concentration of carbon dioxide (CO2) in respiratory gas.The expiratory segment is further divided into three phases (I, II, III), and an occasional phase IV, based on the physiology of carbon dioxide evolution from the lungs and airways: 1 A time capnogram has two important segments: inspiratory and expiratory. Time capnography is used more commonly in clinical practice. Carbon dioxide waveforms can be plotted against time or against expired volume. A decrease in EtCO2 seems to be associated with a higher risk of PEFR ratio less than 50% after treatment.It is important to learn how to interpret the waveform shape to make adequate clinical decisions. Change in EtCO2 from T60 to T0 was associated with a PEFR ratio less than 50%.Īfter 1 h of treatment, there was no significant change in EtCO2. At T60, 20 (36%) patients had a PEFR ratio less than 50%. There was no significant change in the Q angle and the T time after treatment. There was no significant change in EtCO2 after treatment. 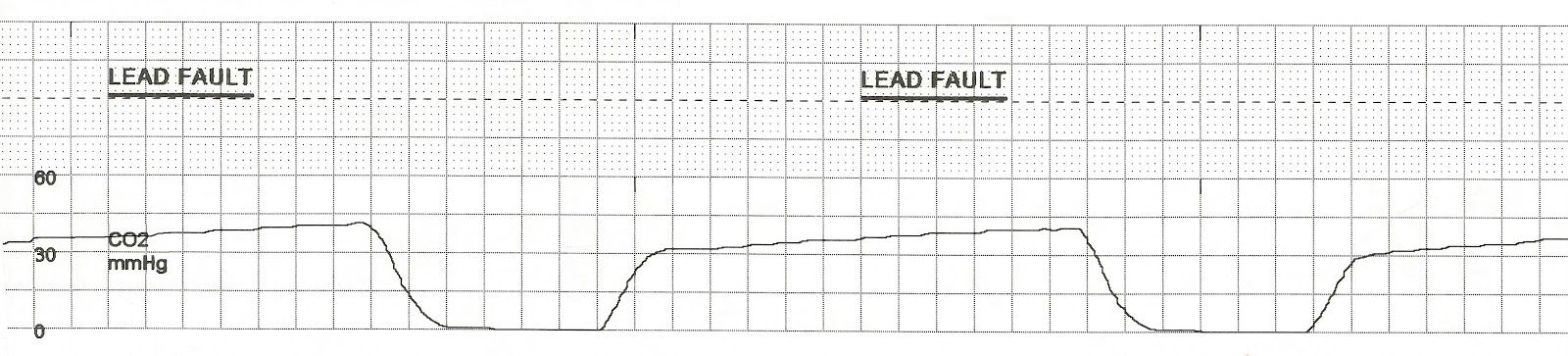
The median initial PEFR was 200 the median EtCO2 at T0 and T60 was 35 (IQR: 30-38) and 34 (IQR: 29-37). The mean age was 37 years and 26 (47%) were women. The primary endpoint was the change in EtCO2 the secondary endpoints included changes in the EtCO2 Q angle value, plateau T time, and change in EtCO2 values for the patients with a PEFR ratio less than 50% after treatment.įifty-five patients were included and 36 waveforms were analysed. Data were collected at first medical contact (T0) and after 1 h of treatment (T60). 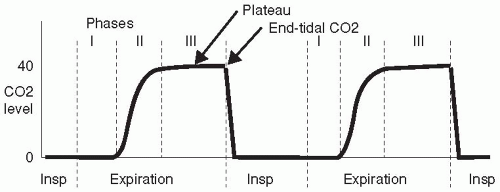
This was a prospective study that included consecutive patients admitted to our emergency department for acute asthma exacerbation. We studied the use of EtCO2 as a monitoring tool in acute asthma. End tidal carbon dioxide (EtCO2) may be considered an accurate surrogate for PaCO2, a severity marker in acute asthma. However, its measurement requires understanding and active participation. The peak expiratory flow rate (PEFR) is the gold standard for monitoring asthmatic patients.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
